The Gut Microbiome: From pre-conception to childhood
Gut health and the gut microbiome and its connection to overall health and disease risk are becoming increasingly popular topics, you may have noticed with the rise in gut-health focused products on the market such as kombucha, kefir and sauerkraut.
But, what is the gut microbiome?
The gut microbiome is an ecosystem of microorganisms that reside in our gut, mostly the large intestine (also known as the colon), these include a variety of bacteria and other microbes – fungi, protists. What many people do not know is that these bacteria have a critical function in our metabolism and digestion and also vitamin and mineral metabolism, immune response with the latest research highlighting its connection to mood too! (Food and Mood Centre).
Some key indicators of a healthy and happy gut microbiome is a diverse range of microbes that provide benefit to our bodies, it is all about the balance! We are still working on accurate technologies to determine the contents of our gut microbiome, however, we know that diet is one of the most powerful factors that modify the gut microbiome. Other modifiers include: antibiotic use, medications, genetics, environmental factors, stress and early life factors – all play a role.
What many people don’t know, is that our gut microbiomes are developed and fully established by about 3 yrs (Tanaka & Nakkayama, 2017). There are a variety of factors which determine how an infant’s microbiome develops and influence their long term health. In this article, the key events involved in the development of the microbiome will be explored. The key stages are during the prenatal period, delivery, infant feeding and the introduction of solids. Other factors including antibiotic use also impact the gut and will be discussed briefly.
In this blog, we will explore the perinatal period, introduction of solids and early childhood and how this impacts the development of the all-important gut microbiome.
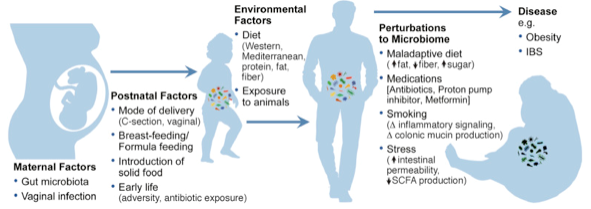
Prenatal period
Collections of bacteria and other microbes live on our skin and also includes the mother’s vagina. Both the mother’s vaginal and gut microbiome undergoes changes during pregnancy. The mother’s vaginal microbiome has been shown to be significant to the development of her baby’s microbiome! The changes in the bacteria at these sites are important due to their role in the transmission of the mother’s microbiome to her baby during vaginal delivery, to protect the baby before encountering microbes in the environment (Mueller, et al., 2014).
Taking a probiotic supplement, specifically containing Lactobacillus rhamonosus GG during and after pregnancy, can help prevent eczema in babies at high risk of developing eczema and allergies (e.g. those with a family history, Szajewska & Horvath, 2018). This evidence emphasises the link between the gut microbiome and immune health.
Antibiotic use in pregnancy has been linked to low birth weight, so antibiotics should be used cautiously and under the guidance of your medical team (Robertson et, al., 2018). For women requiring antibiotics during pregnancy, it may also be worthwhile including prebiotics and probiotics in the diet, while their effects are not conclusive, probiotics have been linked to a reduced risk of preterm delivery (Robertson et al., 2018).
Mode of delivery
The choice to delivery vaginally or via Caesarian section (C-section) is always a parental choice, and of course there are many circumstances where they are necessary and unavoidable. However, the research shown that vaginal delivery is beneficial for an infant’s microbiome development, as it essentially provides the first “inoculation” or colonisation from the mother’s vagina to the baby (Dong & Gupta, 2019).

Babies born via C-section instead receive their mother’s skin microbes, and this is linked to delayed development of their intestinal microbiome compared to babies born vaginally (Dong & Gupta, 2019). This change in bacteria transmitted to the baby has been associated with an increased risk of autoimmune conditions in the future, such as type 1 diabetes, asthma, coeliac disease and allergic rhinitis (Dong & Gupta, 2019 & Tanaka & Nakkayama, 2017).
This has led to many women considering ‘vaginal seeding’, which is the process of applying vaginal fluids on a newborn delivered by C-section to imitate vaginal bacterial transmission of a vaginal birth (Dong & Gupta, 2019).
While this concept sounds promising, it is best to chat to your healthcare team about this if a C-section delivery is an option for you, as the long-term health effects of vaginal seeding are unknown, and may actually risk transferring transmittable diseases to your baby (Dong & Gupta, 2019).
Effect of infant feeding on the microbiome development
The decision to breastfeed, formula feed or mix feed is once again each individual parent’s decision, and breastfeeding may not be possible for factors outside the parent’s control. After birthing mode, whether a baby is breastfed or formula fed greatly affects the development of their gut microbiome. Breastfeeding has shown a clear benefit for microbiome development due to a variety of factors.
One is that breast milk contains prebiotics (oligosaccharides) which promote the growth of a particular bacteria (Bifidobacterium) in the large intestine, which helps establish a healthy microbiome (Tanaka & Nakayama, 2017, Dong & Gupta, 2019).

Breast milk also contains compounds involved in the development of the baby’s immune system (Tanaka & Nakayama, 2017). Due to the unique effects of breast milk on the microbiome, breastfeeding has been associated with a reduced risk of asthma, autism spectrum disorder, and type 1 diabetes (Dong & Gupta, 2019). Breastmilk is also protective for preterm babies against gut immaturity and necrotizing enterocolitis (NEC, Tanaka & Nakayama, 2017). Many hospitals are now offering pasteurised human donor milk for premature babies, a fabulous step forward for women who may not be able to breastfeed and would like for their babies to receive the benefits of breast milk.
For women who choose to formula feed, there are now formulas on the market which contain oligosaccharides to help establish Bifidobacterium rich microbiomes in formula-fed babies, although it does not fully promote a microbiome similar to breastfed babies microbiome (Tanaka & Nakayama, 2017).
Introduction of solids
As an infant is introduced to solids at around 6 months, their microbiome changes to reflect the increased diversity in the diet, and actually allows an infant’s microbiome to develop more like a mature, adult-like microbiome (Robertson et, al., 2018).

The latest research has now shown that breastfeeding duration and a child’s pre-school diet actually play a role in a child’s microbiome composition between the ages of 6 to 9 years of age (Zhong et, al., 2019).
A longer duration of breastfeeding, and childhood plant protein and fibre intake were key factors which promoted a healthy gut microbiome, so prolonging breastfeeding beyond where possible, and a healthy diet during the pre-school years with plenty of plant foods (think veg, fruit, legumes and nuts) is important for healthy microbiome development in childhood.
Antibiotic use in infancy
Antibiotic use in early infancy alters microbiome development, and has been linked to a higher risk of asthma, eczema and type 1 diabetes (Tanaka & Nakayama, 2017). Antibiotic use in infancy is often unavoidable and can be potentially life-saving, however, they should be used sensibly to minimise potential risks.

We know that the first 1000+ days from conception to childhood shape a child’s microbiome potentially for the rest of their life! To promote healthy microbiome development in your child, a healthy diet rich in prebiotic fibres (nuts, seeds, fruit, vegetables, wholegrains and legumes) and probiotics (yoghurt, kefir, fermented products) may be useful, careful consideration of delivery mode, infant feeding choice and sensible antibiotic use in pregnancy and infancy is important, as well as establishing a healthful diet through their pre-school years and beyond.
Looking for ways to improve your diet and lifestyle during TTC journey and pregnancy? Get personalised advice, and apply to work with us one-on-one today – let’s develop a tailored plan to help you reach your goals!
Resources
- Australian Breastfeeding Helpline available 24/7 – call 1800 686 268
- raisingchildren.net.au – Useful resource providing help from pregnancy, to infancy all the way through to teenage years!
- 5 Things You Should Know Before You Are Even Thinking About Trying to Conceive
This blog was written in collaboration with student dietitian Mariam Metwally, who is studying her Masters of Nutrition and Dietetics at the University of Sydney. You can find Mariam on Instagram @tayyibnutirtion